
Your Health Unlocked Episodes
049: Ensuring Financial Health as We Age with The Senior Source
July 11, 2024
---

Deep Dive Articles
Publication Date: January 04, 2023
By: Gloria Slupek, NWHN Member

10 million Americans are currently living with osteoporosis, according to the U.S. Department of Health and Human Services. More than 8 million of them – the vast majority – are women. But what is osteoporosis? Osteoporosis causes bones to become fragile and susceptible to breaking. Bone fractures and the related pain and disability they cause can significantly impact a person’s quality of life, as well as their physical and mental health.
What’s more, osteoporosis treatment has radically changed in a relatively short period. In the early 1990s, women had few treatment options. Now, there are many different types of treatments available. This has created a dilemma for women trying to decide which, if any, of these medications they need as we learn more about the risks and benefits every day.
We sat down with one of these women, Gloria Slupek, a NWHN member so that she could tell us about her journey with osteoporosis. This is her story.
***This interview has been edited for length and clarity***
My name is Gloria, and I’m seventy years old. I’m very active, which is good for the bones. I go out every day and do something. I have a personal trainer, I go for walks, and golf is a particular passion of mine. I’m also taking a few classes at my local YMCA – chair yoga, balance and stability, and cardio, in fact. Movement and connection have always been big parts of my life.

I was diagnosed about 23 years ago. My endocrinologist at the time prescribed Fosamax to help slow the rate of bone loss. I trusted their advice, and I immediately agreed to take the drug.
I was told that Fosamax would help grow bone mass. The doctor said it was like plastering a wall; gradually, the drug would help add to the bone to increase the bone mass. Critically, I was told there weren’t many risks associated with Fosamax, aside from during the first month or so, where there may be some stomach issues, and I should avoid laying down after taking the prescription. The first month passed, and I had no reactions – for years, in fact. Then, eight years later, I was advised to stop taking it because my bone density had improved.
But then, in 2013, I was diagnosed with breast cancer, which complicated things. Part of the treatment for the cancer involved taking a medication where bone mass depletion was a side effect, making medication to mitigate this effect necessary, according to my doctors. That’s when I was prescribed Reclast infusions. I was on those for four to five years but then got off those in a panic as well because I was eventually told that one of the side effects is osteonecrosis of the jaw. That’s a disease involving loss of blood to the bone in the jaw. That wasn’t something I was comfortable with. It sounded pretty scary. So, I switched to Prolia and underwent two courses of treatment until August 2020.
Yes! I continued lifting weights, going for walks, eating right, and doing all the things I could naturally to help with my bones. But then, right before the pandemic started, I was at a golf lesson and noticed a pain in my left thigh. I thought it was muscle pain from my exercises, so I just rested and monitored it for a few weeks. After about a month of it still hurting when I moved, I saw a nurse. This was during the lockdown periods, so it had to be done virtually.
It was the start of a long and frustrating road of discovery. First, the nurse referred me to a physical therapist. When that didn’t do the trick, I began a pain management plan. From there, I was referred to an acupuncturist. Then, an orthopedic doctor sent me for X-rays. By then, my other leg had begun to hurt despite everything I tried. In January 2021, I went for a new bone density test and was then referred to another endocrinologist, who then referred me to a doctor specializing in spines. And that, finally, was when I was diagnosed with the “dreaded black line” in both legs. From the time of my first pain to a stress fracture diagnosis, eight months had passed.
The “dreaded black line,” simply put, is a stress fracture in the bone that, if left untreated, could lead to a severe break. Breaks for people with osteoporosis are very dangerous, as the bones are slow to heal and can greatly affect mobility for the rest of our lives. After my diagnosis, a surgeon called and told me to be very careful for the next few weeks until I could have surgery to put titanium rods into both legs.
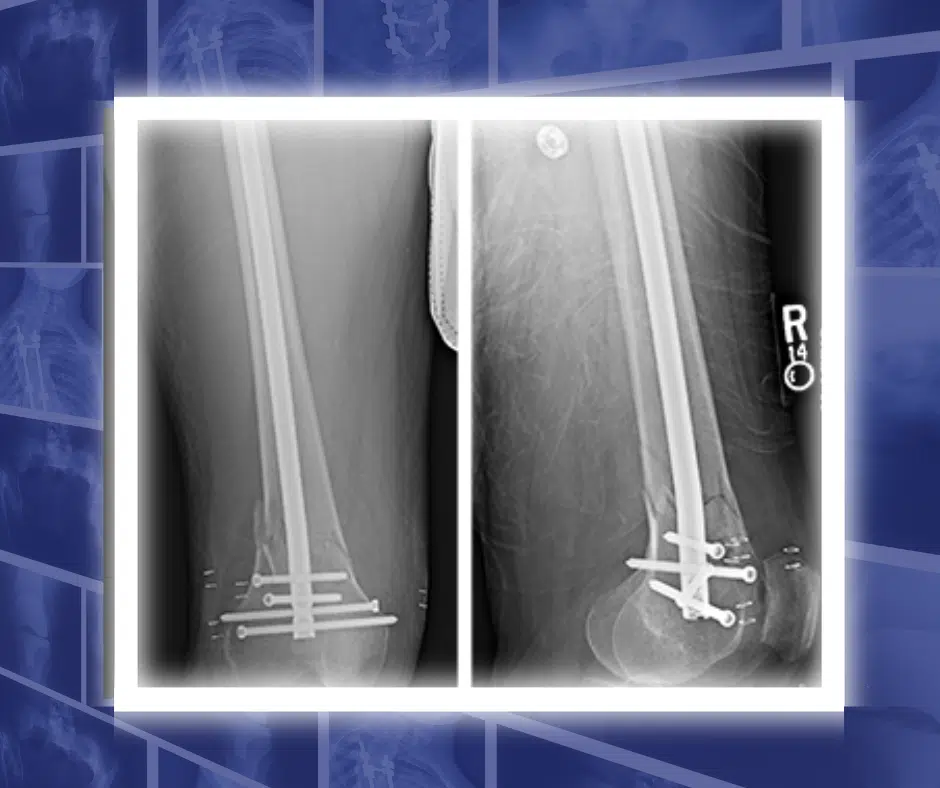
The surgeon assured me that this was the best option and that after surgery, the bones in my legs wouldn’t break because the titanium rods would support and protect them. It made sense to me, but I was reeling. How had I gone from an active woman following every piece of advice given to me by medical professionals – from minor pain on the golf course – to last-resort major bone surgery?
I had the operation for both legs just three days apart.
It was very challenging being incapacitated like that. I had in-home physical and occupational therapy for a month. My daughter had to live with me for several weeks as I needed additional help with basic things – things like showering and getting around my home.
Special equipment was also installed throughout my house to help me get around, including support bars in the shower and a rail support on the bed. I also had to have an extra rail installed to get up and down my three back stairs safely. All of this is at my own expense. I then had three months of outpatient physical therapy. I literally had to learn how to walk again.

My faith and community sustained me. Members of my church would visit and pray with me. And my friends and family supported and helped me throughout. They visited, listened, brought food, and sent gifts and affirmations, which got me through the ordeal.
Yes! I don’t let this slow me down. Today, I live a very full life. I’m back to playing golf, have found a new passion for classes at the Y, and am taking up pickleball. I walk two miles daily and am always working to strengthen my legs. My life is mostly back to normal, but it was a good six months or more of hardship and needing support from health care workers, family, and friends.
They need to be fully informed about the drugs they’re taking to treat osteoporosis and their side effects. From what I understand, the side effects of some of the drugs I was taking started coming to light around 2015, but I wasn’t aware, and my doctors didn’t tell me. It’s crucial women advocate for themselves. That means doing our own research, reading the fine print, and asking doctors lots and lots of questions.
I’d also encourage women to look at non-drug alternatives to building bone mass if it’s possible in their situation. I often wonder if I’d stayed off the Fosomax or the Reclast or stopped those treatments earlier, how my journey would have been different. I have since learned that vitamins B and D, a healthy diet, and exercise are great options for increasing bone density and reducing the risk of fracture.
I also want women to know that you don’t just have to admit defeat and stop moving when you reach a certain age or get a certain diagnosis. I still have pain – I still ache, I take aspirin when I need to – but I also do a lot and enjoy every moment of my life.

Our professional editing staff will work with you to make sure your contribution stands out. And don’t worry – we’ll take our lead from you on things like anonymity, important word choices, and accompanying imagery. Let us help you be seen, heard, and understood. Pitch us by filling out this short form, or just send us an email with your ideas at [email protected].
The information on this site is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. All content, including text, graphics, images, and information, contained on or available through this website is for general information purposes only.
The continued availability of external resources is outside of the NWHN’s control. If the link you are looking for is broken, contact us at [email protected] to request more current citation information.
